The production of egg and sperm cells from stem cells is one of the most fascinating and, at the same time, most complex developments in modern reproductive medicine. This field of research, which is closely linked to stem cell research and reproductive medicine, pursues an ambitious goal: the artificial creation of functional germ cells from ordinary somatic cells. If this approach is successfully implemented in humans, it could fundamentally transform the treatment of infertility.
From Somatic Cells to Germ Cell Precursors
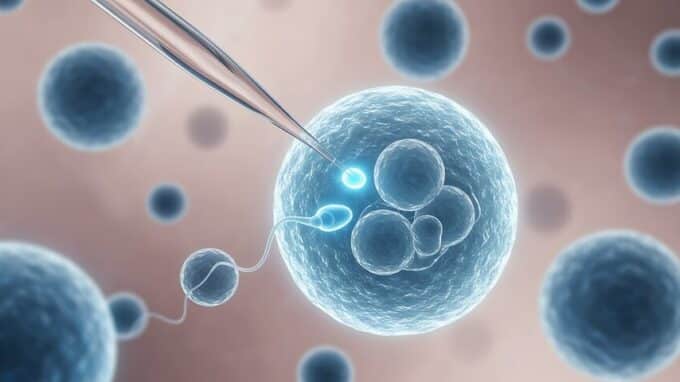
At the heart of this is the technology of so-called induced pluripotent stem cells (iPS cells). In this process, mature somatic cells—such as skin or blood cells—are returned to an embryonic-like state through targeted genetic reprogramming. These cells possess the ability to develop into virtually any cell type. The next step is to convert these iPS cells into so-called primordial germ cell-like cells (PGC-like cells), i.e., germline precursor cells. This process mimics early embryonic development but is difficult to reproduce exactly in the laboratory, as it depends on a highly complex interplay of signaling molecules, epigenetic changes, and cell interactions.
A decisive breakthrough was achieved by the research team led by Katsuhiko Hayashi in Japan. In several studies, he and his colleagues succeeded in first generating induced pluripotent stem cells from mouse skin cells and then converting these into egg cells. These artificially produced egg cells were successfully fertilized and led to the birth of healthy mice. Similar progress has also been made in the production of sperm from stem cells. These experiments are considered a milestone, as they demonstrated for the first time the complete developmental pathway from somatic cell to functional germ cell in the laboratory.
The Challenge of Meiosis and Epigenetics
A key obstacle is the correct execution of so-called meiosis—a specialized cell division process in which the chromosome set is halved and which is essential for the formation of egg and sperm cells. Errors in this process can lead to genetic abnormalities, which is why its controlled replication in the laboratory represents one of the greatest challenges. In addition, epigenetic patterns—that is, chemical marks on the DNA that control gene activity—must be correctly “reset” and reprogrammed so that the artificially generated germ cells are functional.
Despite these difficulties, remarkable progress has been made in animal models. In mouse models in particular, researchers succeeded in generating germ cell precursors from iPS cells and ultimately functional eggs and sperm. These were successfully used for fertilization and led to the birth of healthy offspring. These results are considered decisive proof that the entire process—from somatic cell to functional germ cell—is possible in principle.
New Opportunities for Those Affected
In humans, however, research is still in its infancy. Although human germ cell precursors have already been generated in the laboratory, their complete maturation into functional gametes has not yet been achieved. A key reason for this is that human germ cell development takes significantly longer and is regulated in a more complex manner than in mice. Furthermore, suitable models to safely and controllably replicate the entire development outside the body are currently lacking.
The potential range of applications for this technology is, however, enormous. It could particularly help people who have lost their fertility due to medical treatments such as chemotherapy, as well as individuals with genetically caused infertility. Furthermore, it theoretically opens up new possibilities for family planning, for example for same-sex couples or for people who do not possess their own functional germ cells.
Ethical and Social Issues
At the same time, research on artificial gametes raises a multitude of complex ethical, legal, and social questions that extend far beyond purely medical applications. A central aspect is the safety of the generated cells: Since artificially produced egg and sperm cells undergo profound genetic and epigenetic changes, there is concern that errors could go undetected and be passed on to future generations. Unlike many other medical procedures, potential risks here affect not only the person being treated but also their offspring.
Another important point is the question of genetic integrity and the extent of intervention. The ability to produce germ cells in the laboratory could theoretically also be combined with genetic modifications. This brings the boundary between therapy and targeted genetic “optimization” into focus—a topic closely linked to debates about designer babies and genetic selection. Even though such applications are not currently the focus of research, many ethicists see this as a potential development that must be regulated early on.
Furthermore, the question arises as to who will have access to this technology. Highly complex biomedical procedures are often expensive and initially available only on a limited basis. There is a risk that social inequalities will be exacerbated if only certain population groups gain access to innovative fertility treatments. At the same time, the technology could create new opportunities for previously disadvantaged groups, such as same-sex couples or people without their own germ cells, which in turn would alter existing societal notions of family. The understanding of parenthood and biological kinship could also undergo a fundamental transformation. If egg and sperm cells can be generated from any somatic cells, the question arises as to how “biological parenthood” will be defined in the future. In extreme scenarios, a child could theoretically have more than two genetic contributions, or germ cells could originate from unusual cell sources, raising new legal and social questions.
Last but not least, regulatory and societal oversight plays a crucial role. International organizations such as the International Society for Stem Cell Research are already working on guidelines to ensure the responsible use of such technologies. Nevertheless, legal frameworks vary significantly worldwide, which carries the risk of “regulatory tourism”—that is, the targeted use of countries with less stringent regulations. Overall, it is clear that the development of artificial germ cells represents not only a medical innovation but also raises fundamental questions about the future of reproduction, the definition of family, and the limits of human intervention in nature. A broad societal debate as well as clear ethical guidelines will therefore be crucial for the responsible use of this technology.
Outlook: A Technology with Revolutionary Potential
In summary, the development of artificial germ cells is at a critical turning point: While experimental studies in animal models have already shown impressive success, clinical application in humans is still pending. Nevertheless, all indications suggest that this field of research has the long-term potential to redefine the boundaries of fertility and open up entirely new avenues in reproductive medicine.